About Me
- undergrad RN
- I'm a twenty-something Canadian student. After stumbling through a few years of college, I finally managed to get into the nursing school of my dreams, where I hope to graduate in 2012 with a nursing baccalaureate degree. I want to offer an honest look into how a modern nurse is educated, both good and bad. Eventually I hope to compare my education to my day-to-day career and see how it holds up. Whatever happens, it should be somewhat entertaining. Find me on allnurses.com!
Google+
Blog Archive
-
►
2008
(87)
- ► February 2008 (9)
- ► March 2008 (1)
- ► August 2008 (10)
- ► September 2008 (13)
- ► October 2008 (20)
- ► November 2008 (12)
- ► December 2008 (6)
-
►
2009
(40)
- ► January 2009 (12)
- ► February 2009 (5)
- ► March 2009 (8)
- ► August 2009 (6)
- ► September 2009 (1)
-
►
2010
(53)
- ► March 2010 (2)
- ► April 2010 (10)
- ► October 2010 (11)
- ► November 2010 (9)
- ► December 2010 (10)
-
▼
2011
(50)
- ► January 2011 (10)
- ► February 2011 (10)
- ► March 2011 (4)
- ► April 2011 (5)
- ► September 2011 (4)
-
►
2012
(3)
- ► January 2012 (1)
- ► February 2012 (1)
Hey, You! Spam Guy!
Scattergories
- about me (18)
- articles (3)
- becoming a registered nurse (1)
- becoming a student nurse (13)
- blogging (19)
- books (6)
- care plans (1)
- certifications (2)
- classes (14)
- clinicals (28)
- CNSA (8)
- conferences (13)
- cool stuff (7)
- diva cup (2)
- emoting (24)
- equipment (5)
- exams (26)
- family (1)
- friends (8)
- group work (13)
- horses (5)
- life outside school (14)
- memes (4)
- military (3)
- money (2)
- More tales from the ER (12)
- people i admire (12)
- politics (1)
- post-grad (2)
- preceptorship (2)
- profs (17)
- projects (6)
- reflecting (16)
- resources (9)
- reviews (2)
- scholarships (2)
- Sigma Theta Tau (3)
- snark (11)
- studying (10)
- technology (10)
- travel (1)
- UNE (23)
- uniforms (4)
- volunteering (1)
- Weight Watchers (1)
- work (19)
- workouting (6)
- WTF (3)
National Informatics Project!
One flu (vaccine) over the cuckoo's nest
I'm about halfway through my nth shift delivering flu shots to the masses. Although it is monotonous at times, I've actually found it to be a pretty good experience. I work casual hours which means I can pick up shifts as I like, and I can even cancel a shift if I get too bogged down in school work. I've met all kinds of people, and gotten semi-decent at small talk. I've also developed a mighty smooth IM technique!
Things I've learned from flu clinics: I have absolutely no desire to work with children. Even if the kids are behaving perfectly appropriately for their ages, I find them stressful. Let's not forget the parents who try to convince me that their 7 year old sniveling kid will sit still by himself for the shot.... Not falling for that one again!
I actually find the flu clinic kind of an enjoyable escape from emergency. After the first week, most sites have been VERY quiet. My stress level right now is about -10. After my high-stress city job and a summer in emergency, I almost feel guilty that they pay me to do this....... Alllllllmost :) my favorite part about this is that no one treats me like "a student" here. I'm a member of the staff, I do my own thing unless I have a question. I can make normal conversation with the nurses, for probably the first time ever. It's great.
In other news, it's about 3.5 weeks away from the end of the semester! this semester has been RIDICULOUS. I was walking to school this morning in the pitch black cold and I thought to myself.... Man, 4 years is a long time. I've been standing on this same sidewalk waiting for this same light to change in this same crappy weather holding a coffee from the same Tim's since 2008.
The workload has been a steady insane pace for the last 2 months, and it's shifting into overdrive for the rest of this month. I have 2 more group presentations, 3 more papers, and a bunch of quizzes and minor assignments to complete by December 2. I also have to finish my oncology nursing certificate by the end of November, except that's impossible so I will have to extend it until January.
BUT. And here's the big but.
I have my preceptorship placement confirmed!
I am going to Oncology!
I am so excited!!! The cancer care center here is huge and highly respected. I also had such a good experience with the oncology nurses that I met at the CANO conference in Halifax. With any luck, I will knock their socks off, and be offered a full time line after I am done my preceptorship hours. :)
Assuming I like it there, of course. But I am feeling very, very positive about it.
Honestly, after some months away from full time emergency, I'm starting to wonder if there's a better fit for me. I mean, emerg is AWESOME experience and I can't say enough about the expert knowledge there. The nurses are mostly super kind and helpful. I will absolutely stay there on a casual basis. But, something's missing.....
.... The kind of relationship building that you get with inpatients. The chance to see the results of your hard work. The possibility of being on a first name basis with your client in a real kind of way. The opportunity to really, really talk about health promotion with your clients, the kind of deep talk that happens at 0-dark-thirty.
I mean, those things do happen in emerg, but rarely. The norm is that I'll round on a patient 2 or 3 times and then they'll be discharged. The ones who come back, our lovely frequent flyers, don't usually come for the witty banter or healing presence of yours truly ;)
I guess it's that some of my classes this semester have struck a chord. Especially in my Chronic Conditions class, we really talk about primary health care, and I want to be more involved with my patients in that kind of way. Obviously inpatient Oncology isn't really the place for that. But it's got a chance for that kind of relationship building, and I see a lot of opportunity for primary health promotion at the community level.
I've got my orientation for the hospital at the end of November, and I'm super pumped. It's for the inpatient-side, so I guess that will be a lot of the really-sickies, palliative care, that kind of thing.
Can't wait! Getting so close to real nursing!
That's So... Meta
So early in my nursing school adventure, I daydreamed about what the upper-level classes would be like. Well, not really the 400-level courses since they seem kind of dry by title alone: Future Directions of Nursing, Leadership, Bioethics of Health Care. I was so excited about the 2nd and 3rd year stuff. Lab skills, patho, assessment. I remember, shortly after I was accepted into the program, staring at the curriculum and wondering who and what I'd be like once I'd gotten to where I am now. I remember seeing myself in some nebulous idyllic clinical representation, the essence of confidence and expert nursing skills, making effortless profound impacts in the life trajectories of my patients. Hahaha :)
Well, as you know if you've been here or if you've read my blog for any length of time - there's really no such thing as effortless at this stage. I overthink the hell out of every move I make, either before I enter the patient's room, or as I lie awake in bed wondering if I did or said the right thing. My romantic ideas of nursing are muddied further by challenging instructors, complex work-school-life balancing, and learning to navigate coworkers and professional relationships.
Anyway, I guess I'm trying to say that my reality is both laughably departed from what I imagined, and in some ways exactly what I hoped it would be.
So that brings me to this year. These courses which I just viewed as the last necessary steps to my final placement and -at last!- status as Registered Nurse. I thought this semester would be the longest one of my life.
Nothing could be further from the truth.
I LOVE this semester and everything about it. We're already 4 weeks in, with 9 weeks to go before finals. Through divine intervention, or a reasonable facsimile, all of my classes have amazing instructors, including some of my favorites from years past.
The biggest difference this year from previous years is the distinct lack of rote memorization. I don't have any lame keywords to memorize for the final. It's like we spent the last 3 years learning (and forgetting a lot of) that kind of micro-knowledge. My lectures this term are all big-picture discussions. We don't spend so much time convincing each other what nursing's supposed to be (since none of us actually know, anyway). We actually talk about realities of nursing, as seen through our experiences in clinical and as UNEs. Macro stuff like is this congruent with what we imagined? Where is nursing as a profession, and where do we think it should be?
Another thing I love is how empowering my instructors are. They are always reminding us about who the future of nursing is, and how it's up to us to make it into what we think nursing needs to be.
I leave every class with my mental wheels turning. I've been known to jokingly complain to my friends about how META my classes are. Seriously, this semester makes me so happy! I think it's shaping up to be my favorite one out of this whole program.
Right now I'm working on my first paper for this term. It's a review of a pop-lit book on leadership. I'm reviewing the book "Primal Leadership" by Goleman. It's kind of a long-winded project since I have to finish the book before I start the paper (due Friday), and amidst my already packed reading schedule it's been kind of a grind.
In other news, I will be working the flu immunization clinics this year. Orientation for that is on Thursday. I fully expect to be amazing at IM injections by Christmas ;)
Thanks to those who added me on Google+ so far! You rock :D
Yayfriends!
So you might have noticed that I've set up this blog to have its own (experimental) Google+. If you're down with getting conversational, add me! Please include a non-creepy note so that I know you're a real person and worth saying hello to :) Also, let me know if you're a nurse/student/allied health professional or if you do something else we can talk about! If you're extra not-creepy maybe I'll consider adding you to my real Google+, but that's more of a long term kind of thing <3
A Summary, a Conference, a Project, and an iPad
I really have to apologize for the dearth of posts lately. I've got no good excuse except for the usual premium on spare time that comes with nursing school. So that aside...
A Summary: I really want to talk about my experience as a UNE (student nurse extern) in the ER over the summer. I freaking LOVED it. On speaking with some of my classmates, it seems that I got pretty lucky in my placement, because my particular ER is small and ultra-inclusive - there simply wasn't enough help to go around, so I was always considered part of the team, and like an extra set of hands. Turns out some other people placed on Med-Surg/postpartum were viewed as subpar RN stand-ins. As student nurses we are mandated to take a smaller patient load and lower acuity than staff nurses - which makes sense. Yet some of the staff nurses took the perspective that the UNE had it easier and so made their jobs harder, where other nurses saw us as a bonus to the existing staff and as lightening the load by taking a patient away from each of the other nurses.
So I am even more grateful that I had such a positive experience this past summer. I was on the unit from May through the beginning of September. My scope was pretty big. There were a few things I couldn't do at all or without RN supervision, and some of my meds needed to be cosigned, but I worked really hard and helped out a lot. I almost never sat down except for a quick charting session. It got to the point where I was starting to anticipate the flow of the ER and what might be done for certain patient presentations. I asked questions and clarified interventions. I saw several urgent presentations and maybe even a couple of emergencies, although I still haven't witnessed a code or done CPR on a human. I made real differences to several patients. I learned how to work as a team, contribute, and COMMUNICATE. I made more money on shift differentials then I ever expected (woo night shift!!) - but, most importantly to me, I gained so much experience in the nursing role and, like, quintupled my comfort level with all the psychomotor skills that made me so nervous in lab. I saw so much this summer.
Some of my coworkers were more difficult than others to really learn from. One in particular struck me as an exceptionally competent nurse, very confident and knowledgeable, but she was like a prickly pear to talk to. I guess like your typical Type A ER nurse (for the record, I'm pretty much a Type B introvert, and I still enjoyed the ER, so don't let anyone tell you otherwise). I got a lot out of shutting up and watching her, but forget asking her any questions, she didn't have time for students. Or so it seemed. And there was the charge nurse who wasn't the best teacher. But the overwhelming majority of my RN/LPN coworkers were super kind and patient with me. They all made such an amazing difference in my practice and I told them so!
Would I recommend Alberta nursing students be a UNE during the summer after 2nd and 3rd year? Unequivocally YES. It's like nursing school on speed. You'll start making sense of the theory in ways you didn't expect. You'll gain the psychomotor skills to actually do lab skills on real patients without your instructor hovering over your shoulder, and while you do those skills you'll start to work patient teaching into your practice. Then in 4th year you'll have real-world examples to back your shit up when you write papers. Or blogs.
A Conference: I was the fortunate recipient of a travel bursary to the CANO annual conference in Halifax, NS. There was supposed to be another student who went, but I never met her.
In a nutshell, Oncology Nurses are seriously knowledgeable. They are also awesome because, from what I experienced at this conference, they are valued as collaborative and worthy team members even by physicians (kind of a hard status to come by, it seems) and are extremely supportive of complementary/alternative medicine (CAM), not so much because of the evidence surrounding CAM but because patients want it and find relief from it, and they need their primary providers to be open and knowledgeable about it too.
The conference was 4 straight days of learning. Corporations sponsored almost all of our meals, and during each meal there was a presentation on some new wonder drug or different approaches to patient care. There were also a multitude of workshops to attend, where nurse researchers would present their latest abstracts and findings.
I had a lot of difficulty integrating myself into the conference because, as specialists, the presentations were operating at a pretty high level of comprehension. The conference attendees were almost all advanced practice nurses - NPs, CNSes, and tons of nurses in research and academia. They would debate different chemotherapy drugs and weigh the pros and cons, and things like that, which was kind of meaningless to me as a student. There was some stuff I did learn a lot about, such as a yummy dinner symposium at which we learned about treating clogged CVADs. I don't remember learning much at all about CVADs in class. The dinner was beef and chicken. The beef was served medium-rare, and pretty pink/fleshy in the middle. It was at that moment the presenter posted some photo examples of blood clots extracted from CVADs. They looked eerily similar to my beef dinner. At which I thought, "Only nurses would be totally cool with watching this as we eat..." mmmmm :)
Another challenge I found was the huge jump, not only in experience, but in age between myself and the other attendees. Being as they were almost all out of bedside nursing (and with the commensurate experience), I'd peg most of them as 40+. Not that there's anything wrong with being 40+. It just didn't give me much to talk about with them. So most of the time I would sit down with a new group of people at a table, introductions would be made, and they would ask me where I worked.... when I would say "Oh, I'm a student".... and the conversation would awkwardly shut down or divert amongst the RNs. It made for kind of a lonely time at the conference although I did meet and network with lots of people. I even met the lady who does the clinical placements for our local Cancer Care centre, where I am hoping to get a placement for my preceptorship.
The CANO BoD contacted me after the conference and wanted to get my perspective as a student attendee. I think I will recommend that they try to designate a "Conference Guide" for future conferences, who can assist the students to really understand the presentations and kind of bring it all together. I think I would have benefited from some kind of debriefing.
On a totally positive note, several of the nurses I sat with were really pleased and happy to help me understand the presentations. I could see that a lot of them were probably involved in teaching. So that was really kind and super helpful. I got a ton of notes from all the presentations, so I might be able to review them once I am practicing and maybe they'll make more sense. :)
A Project: Through my work with CNSA as Informatics Officer, I have been working with CASN and CNA on developing informatics competencies to add to curricula for undergraduate nursing education. I think it's cool that I'm working alongside some heavy hitters in academic and professional spheres on a project that will impact the future of nursing education in Canada. At our teleconference in August, we needed to elect a chairperson for our committee, and some of them suggested that it would be a good experience for me. I think so too, but I really don't know what I'm doing as a chairperson. I told them that if they were patient with me I'd be happy to take on the role. Part of this means I will be presenting our findings to a stakeholders' symposium in Toronto at the end of November. At our last teleconference I discovered who would be considered a stakeholder. I'm super pumped/terrified to meet these people, but wow, what an opportunity.
An iPad: It's no secret here or anywhere else that I have a special fondness in my heart for Apple products. I was one of the original hires to help open the first Apple store in Western Canada (which was a pretty fun day! :). The love is waning a little bit with Apple's continued pricing structure, surging popularity, and militant control of how I enjoy my products, but, on the whole, I still can't beat the user-friendliness of iOS/OSX. Can't argue with the fact that after I convinced 4 of the family members who called me all the time with computer issues, I don't really have to troubleshoot anyone's crap anymore, because it doesn't need troubleshooting.
So when I saw the reading list for this semester, and noticed how much of it was PDF academic articles, I winced and wished there was some way I could read these in a more comfortable manner. I really try to avoid printing anything because I am cheap and scatterbrained. I also hate reading articles on my laptop because of i) the searing pain in my lap once my computer's been on for >20 minutes, and ii) I am way too easily distracted by Spaces.
So I started checking out some different kinds of tablets. Initially I was intrigued by Samsung's Galaxy 10.1 since I might be converted to Android. I certainly am willing. Anyway, after lots of research and playing with tablets at Best Buy, I decided the extra $50 or whatever was worth the negligible decrease in performance/portability/resolution in exchange for an exploding App Store and seamless integration with my existing tech setup.
Anyway, I bought the iPad last Saturday on an extreme trial basis. I had very specific criteria in order for any tablet to be superior to my laptop. I was/am ready to return it if it didn't work for me:
1) It had to be incredibly easy to integrate with my cloud server on Dropbox
2) Accessing and editing documents on Dropbox had to be seamless
3) Accessing and editing PDF articles and class notes had to be comfortable and realistic (nothing too complicated)
4) Google Calendar had to play nice with iCal or an acceptable equivalent
5) There had to be apps out there to make it superior to my browser-based existence
6) OSK is just not realistic for me, so I wanted a great/portable Bluetooth keyboard
Today is day 5, and honestly, I don't know how I got by without it. I LOVE curling up in bed, locking out the rotation, and reading/annotating my PDF articles or even just web browsing or watching Netflix. I am beyond impressed with how most software seem to integrate with Dropbox or other cloud servers.
Right now I have been using Goodreader to read/annotate PDFs, Quickoffice Pro HD to view/edit my Word/Excel docs, and iProcrastinate to manage my workload. Unfortunately iProcrastinate only has an iPhone app at this time, but it syncs up with my Macbook so it's all good. So nice to be able to see what's coming up next between all my classes.
Tomorrow I will try AudioNote especially in my Philosophy class. The prof is very much a talker, and doesn't tend to summarize her points in any logical fashion, so I think recording her lectures and having them timestamped to the notes would be a great thing. We'll see how it goes.
I have been finding a lot of apps that might be suitable to nurse-types, so I was thinking I might do a review of these in the future so you can get a feel for it without shelling out money.
As far as the keyboard setup, I was heavily swayed by NNR's review of ZAGG's keyboard. I checked out Future Shop and found one open box, missing the USB cable. Since I have a few of those anyway, I sashayed up to the sales guy and asked him to "make me a deal" on it complete with flirtatious lashes. He knocked off another $20(!) for me, dropping the price from $100 to $75. Excellent. I love the keyboard, too, although it's good that I don't have man hands, because the keyboard's certainly petite. Together with the iPad, it still weighs roughly 2/3 less than my Macbook, not including the charging cable, and it definitely takes up much less valuable space in my bike pannier.
So altogether, between the cellular data, the apps, the cloud integration, and the ZAGG keyboard, I am quite pleased with my setup. Bonus points for form factor, weight, battery life, and lack of hard disk drive. I will continue evaluating right until Saturday of next week which is the end of the allowable return period.
Anyway, I have been blogging away from yet another new app - Blogsy. I really like it. Even better than I like Blogger's old back end. I used it to write this blog post - I am hoping that the improved mobility will make it easier for me to blog when I have the desire instead of waiting for when I have time at home with my computer.
I guess that about covers everything. For now. :)
It's here! Fourth and final year!!
It's crazy to look at my syllabi and see all 400-level courses.
This fall semester is my final lecture-based term; Jan-Feb is my consolidation and then Mar-Apr is my PRECEPTORSHIP!
I put in my preceptorship placement requests yesterday after a lot of serious thought. Basically, after much deliberation and longing to try every specialty but being restricted to only 3 choices, I finally decided on Oncology, Cardiology, and Corrections.
A few that fell on the cutting room floor were PACU, ICU of all types including CCU, public health particularly women's sexual health, and a brief daydream of something extra crazy like OR. I also didn't consider asking for Emergency since I wanted to try something new.
Why not critical care? Although I'm tremendously interested in it, and I KNOW I'd learn a lot, I spent a lot of time reflecting on the criteria to excel in my preceptorship. Some of those things include initiative, the ever-elusive "critical thought", and transitioning to a grad nurse role. I honestly don't think I'd be able to excel in those criteria in ICU. Yeah, a 10-week preceptorship would be an awesome orientation to the floor, but really, it would just be an introduction. In my final preceptorship I'm expected to be a grad nurse. I feel like I'd spend so much time being a fly on the wall, I'd be too afraid to get in and get my hands dirty, so to speak.
The choices I picked are ones that I think have opportunities as a newbie nurse to actually show some initiative and capability as a health care provider.
We had to provide some rationales for our choices, and these were mine:
1. Oncology: My interest in Oncology stems from both the prevalence of cancer diagnoses across all patient populations as well as my family’s experiences with cancer. I feel uniquely prepared for a preceptorship in oncology nursing as I am currently completing the ONDEC course through the Alberta Cancer Board. I am also a student member of the Canadian Association of Nurses in Oncology (CANO) and will be attending the CANO conference** in Halifax this September to learn more from dedicated Oncology Nurses about their specialty. In return for receiving a travel grant, I have agreed to write a journal article for one of CANO’s publications and I am hoping to write about my preceptorship experience and transition from theoretical knowledge into practice as a graduate nurse.
2. Cardiology: I have worked as an undergraduate nurse in the Emergency setting over the past summer. I have tremendously enjoyed working in the ER and have found that one of our major patient populations are either experiencing acute cardiac changes or have a history of cardiac/vascular pathophysiology. Having worked closely with several former Cardiology nurses, I admire their extensive knowledge of this specialty. As I have been invited to stay with the ER after I graduate, getting first-hand experience with this specific population will be extremely educational and give me confidence when working with new-onset cardiac concerns in the ER. My RN coworkers have commented on my willingness to get involved and ask questions to further my understanding, so I believe I could meet the required objectives to excel in this placement.
3. Corrections: My first post-secondary program was in Policing, of which I completed 50% of the course credits. I still have a strong interest in law enforcement although I am geared more towards prevention and rehabilitation rather than apprehension. At the ER we also had several inmates transferred to our facility for treatment. I believe that with my educational background and ability to respect and work with corrections patients without judging their histories, corrections nursing would be a unique opportunity to make a positive impact in an underserved population.
**In other news, as you read, I am going to yet another conference! There are just so many opportunities for students to get involved in Nursing. I have some other projects I'm excited to tell you about. But that post will have to wait until, at least, I get a decent night's sleep :)
WaHOOOOoooOOO FOURTH YEAR!!!!!!
Loss of a Statesman
Check, check, checking out
There were the usual WTF visits, like the mom who ABSOLUTELY had to get her kid "tested" for celiac disease in the middle of the night. At the ER. Where people were practically hanging from the rafters in the waiting room. The urgency? Well, she Googled a new diet and wanted to start him on it the next morning... "Can't I just see the doctor real quick?"
"No. I'm sure the other 25 people in the waiting room would like to see the doctor 'real quick', too." Then, after lipping off the triage nurse, she stormed out. Bye...
 |
| medscape.com |
It's 0430, do you know where your soldier is?
I don't necessarily believe in what the military *does*, but I do support the men and women who stand up for their country in one of the most honorable ways possible and the sacrifice they make in that choice.
But I think the sacrifice goes far beyond a tour of duty and service on the front line. I think that the military completely fails its troops once it's time to re-enter civilian life. In absence of psychological intervention, soldiers turn to any variety of things to numb their thoughts and dreams, and too many of them end up dead.
Thanks for serving your country, here is a sense of manly bravado, zero coping skills and tons of bad shit to deal with. Bye bye now!
Seriously, so sad. I just want to go all "The Cell" on him and hop inside his mind and bring some peace there.
-- from the cellular desk of undergrad RN
Got angry at/for a patient...
A young woman was brought in by police a self-inflicted laceration. At first it just seemed like your run-of-the-mill angsty teen cutting.
So I brought her in, pulled up a chair, and said..... "start from the beginning".
And she talked, and I listened, and she cried, and I held her hand.
 |
| http://www.twloha.com/vision/ |
"But don't write any of that down," she said. "My hormones got the better of me. I was asking for it."
I told her about her resources and her options, but she didn't want to hear it. She didn't want to acknowledge that her husband laid his hands on her, hurt her, scared her. Hurt her so much that she told me "if he hurt me, why shouldn't I hurt myself?" and she cut herself to cope.
I know family violence happens. I know that women statistically have to ask for help 7 times before they commit to a change... but part of me just wanted to shake her and say "you can do better than him! He CAN'T do that to you!"
I know all that but I still wanted to go and knock him out. I was really upset and talked about it with my fellow students and nurses, but man. I'm really bothered by this one.
At the end of it, I told her that if she EVER felt like she had nowhere safe to go, she could come to our ER and we'd take care of her. She burst into tears. What more could I say?
You need to know that rescue is possible, that freedom is possible, that God is still in the business of redemption. We're seeing it happen. We're seeing lives change as people get the help they need. People sitting across from a counselor for the first time. People stepping into treatment. In desperate moments, people calling a suicide hotline. We know that the first step to recovery is the hardest to take. We want to say here that it's worth it, that your life is worth fighting for, that it's possible to change. - To Write Love On Her Arms
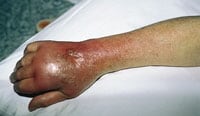
Looks like chicken
I was struck by the whiteness of the bone. Looked like a chicken bone.
| http://bareessentialssportsmedicine.com/ |
The dislocation was reduced, the lac was sutured, and I think the pt was referred to an orthopedic surgeon and/or plastics for follow up.
More tales from the ER...
A nurse's day in the ER
I love nursing.
Now onto the good stuff.
In our ER, all the shifts are pretty much the same. The only differences between days, evenings, and nights are the volumes of patients and the amount of sleep you get. For convenience, I'll describe a day shift.
0715: Oncoming nurses arrive. This hospital hires LPNs to cover peak periods at night, and UNEs during the summer (like me!); otherwise all nursing staff are RNs. Oncoming nurses are laden with junk food and Tim Hortons coffee.
0730: We gather at the nursing station for report. The off-going charge nurse gives report to the oncoming charge. She pulls up the electronic ER management program on the computer which shows a map of the ER with names, ages, triage scores, and triage notes for the admitted patients in their respective rooms. She goes over every patient and mentions pertinent details: when and if they've been seen by the MD, lab and x-ray results, precautions, assessment details, and discharge planning. The ER truly is the kind of place you start planning discharge as soon as they are admitted (mostly: how are they planning to get home?)
0745: Report's finished, so we clear out of the room so the off-going nurses can grab their stuff and go home. We gather at the charting station and scan over the charts there. Sticky notes are posted to each of the charts to remind us when the next set of vitals are due, what the last chem strip (aka blood glucose) was, or whether we need to hang a second bolus after the first one's finished. We usually check vitals q2h.
0800: V/S are all caught up and the unit clerk puts up a chart in the rack for Team 1, which is one side of the ER. Team 1 has 3 different nurses, and I float between Teams 1 and 2. So, whoever is on that team (or floating) and happens to be near the rack at that time will take the order, and this time it's me. I grab the chart and put on my MD-handwriting-analysis goggles. I decipher that the patient is to receive 30 mg of Toradol IV. I scan the initial assessment and see that the patient was admitted for back pain. No allergies to NSAIDs. I quickly check the previous orders and see that she has a 1L bolus of normal saline running already. Since I can't give IV push medications, I decide to hang a mini-bag secondary infusion. I check the parenteral manual and see that it can be diluted in 50 mL of N/S and calculate the drip rate. I head over to the Pyxis and pull out a vial of Toradol 30 mg/1 mL, do all my checks (I'm OCD about checks - terrified about med errors). I mix up the bag, label it, and prime the line. I head into the room, explain the med, do my final checks and then hang the mini-bag.
0825: Another order's up. It's a discharge for the patient in room 2 with a tooth abscess. She's to get 2 Percocet tabs now and 5 "to go", which means we send them home with PRN instructions. She's also got a prescription for Keflex and a referral to a social worker, which I interpret to mean that she probably can't afford a dentist. I pull the Percocet and put 5 into an envelope with instructions to take 1-2 tabs every 4-6 hours for pain. I bring the meds and give her our narcotic info sheet to sign. It basically says that they are not to drive or make life-altering decisions under the influence of narcotics. I explain the PRN instructions and give her the Keflex prescription, giving a quick and dirty explanation of the importance of taking all the antibiotics. I discontinue her IV and send her home. I quickly strip the bed, wipe everything down, and put on new sheets for the next person.
0845: So we now have an empty bed with 10 people in the waiting room. Room 2 is a "general use" kind of room (it doesn't have any specialized equipment), so I head to the rack at triage and pick up the next chart. It's a little boy who presented with a temperature of 38.9°C, with a dry cough, sore throat. He was given Tylenol as per the triage fever protocol, so I call him up and reassess his vitals before bringing him back. Temp's down to 37.5 (yay!) and I bring him and his mom into room 2. The little boy is "ILI positive" (influenza-like illness) and I place them on contact and droplet precautions. I chart my preliminary assessment at the bedside - antipyretic medicine effective, skin warm and dry, back of oral cavity is red and child c/o pain on swallowing. Neck nontender on palpation. Immunizations are up to date. Child is voiding regularly. Eating and drinking with no nausea, vomiting, or diarrhea. Mom was concerned because he had a history of febrile seizures and thought she should get him "checked out". Child has no allergies or medications that he takes regularly at home. No previous medical history except for the seizures.
0910: I head to the charting station and complete the chart and nursing notes, and report off to Team 1 on this new admission. There are no new orders so I catch up on reassessments on the admitted patients.
0930: No new orders, no patients to bring back, and the waiting room has 13 people in it. I head up to triage to help reassess those patients still waiting. The computer assigns timers to each of the triage code, so higher-acuity triage scores get flagged for reassessment more frequently. The trouble with reassessments is that people hear their name and think they are going into the back. They don't like returning to the waiting room. Another nurse tells me to call them up as "Mr. Franklin, for REASSESSMENT!" and set expectations from the get go. I get through about 5 reassessments and we are all caught up. I don't like sitting at the reassessment station because it faces the waiting room and I get evil death stares from the patients, and lots of people who think the ER is a turn-based facility and get angry when people go straight back from triage. I have a long history in customer service and it feels very, very good to let the customer know they are not always right.
1030: Break time! I get 30 minutes. I occasionally ride my bike to Tim Hortons for a steeped tea, yum! Before starting in the ER it was hard to convince myself to actually take breaks - too much to do, too much to see. I'm starting to appreciate them now, though ;)
1110: The charge nurse urges me to duck into the trauma room where a young person is getting an I&D on a massive leg hematoma. The MD uses procedural sedation and then incises the top of the wound. He laughingly tells us gawkers to stand clear because we could get hit with the spray. Between much bubbling, gurgling, and massaging, copious amounts of old blood and black clots come popping out of the wound. Amazingly, there is no smell to it. The MD packs it with not one but TWO full bottles of packing. We clean up and I dress the wound. The patient's leg is about half the size. It is amazing what the human body does.
1205: I pull Gravol and morphine to administer IM to a woman who scalded herself with the deep fryer. I am amazed at how quickly I can landmark ventrogluteal injections now. She doesn't even flinch, I'm not sure if that's a compliment to me, or a sign of how much pain she's in.
1235: A young guy is wheeled back from triage, after presenting with a sore head and neck after a MVC at 80 km/h. He was t-boned by a truck that ran a stop sign. He needs an IV started and I get all excited because he's under 30 and a weightlifter.... therefore great veins. I dash into the room with the IV cart. It still takes me forever but I am pleased to hit a vein on the back of his hand with minimal discomfort to him (or me). A senior nurse was waiting to push some morphine and she said she was pleased with my technique. Anytime a nurse with that kind of experience has something kind to say about a nursing-related topic, I always look over my shoulder wondering who they're talking to........
1305: A volunteer is wandering around the department looking bored. As a previous volunteer in this very ER, I know *exactly* how they feel. I make a point of delegating fun-yet-simple tasks to them. Please: Escort patient to x-ray. Make soup and toast for room 10. Clean suture tray from the trauma bay. I like talking with the volunteers because a lot of them aspire to be where I am - on the payroll :)
1340: Reassess vitals, hang new IV solutions, push meds, run ECGs as necessary. As a UNE, I'm like the go-to helper person. I can't do everything that an RN can do but I am an extra pair of hands.
1400: Break time! I have lunch in the break room with some of the newer grad RNs. Several of them were UNEs like I am now, and they came back to work in this ER because they loved it. So do I.
1435: A guy walks in from triage. Chest pain since last night. Patient is a 49 year old male, overweight with a lot of abdominal fat, diaphoretic throughout the night, family history of acute coronary syndrome. I get him into a gown and run an ECG on him. I'm not very good at interpreting rhythms, but even I can see that the time elapse during the QRS wave is loooonggggg. I don't know much but I know bad when I see it. We move him into the trauma/code bay. MD says it looks like an NSTEMI. The RNs begin the heart response protocol and get multiple IV accesses. Someone thrusts a bottle of nitroglycerine at me to hang. I've never hung a bottle before. I poke at it a couple of times and then give it to an RN to show me how it's done. I can, however, prime a N/S line, so I do that while I watch. Once his lines are in, I stand by the chart and write down all the stuff as it's called out - vitals, new line insertions, nitro drip started at 1450, etc.
1525: Oncoming shift has arrived! They pile into the report room.
1530: The unit clerk has booked transport for the NSTEMI to be transferred to a cardiology unit at a major hospital. In the meantime I round on the other patients. It's amazing what a warm blanket will do for someone who feels like they've been waiting too long.
1535: I finish rounding on all of the admitted patients and make sure everyone is looked after before shift change.
1540: Transport arrives. They pack the patient into the EMS stretcher, receive report as they secure him, and roll him out. I clean the room, ready for the next patient.
1545: I head home, and the next shift begins....
Target Practice
[mini-rant]
I wish that laypeople would stop using the "IV Experience" as the sum evaluation of their interaction with nurses. How many times have people found out that I'm in nursing school, only to launch into a tirade about their latest hospital stay -
"I had a terrible nurse! She had to poke me with the IV TWICE!", or
"This one nurse was useless, she couldn't get an IV started, so she got another nurse who got it on the first try!", or
"The last time I was here the OTHER nurse had no problem.", or
"The nurse got it in but she must have done something wrong because now I have a BRUUUISE" or,
"My nurse was great. She got the IV started and I barely felt it."
How many other factors are involved here? Location, skill, gauge, hydration, BLIND LUCK? Seriously!
[/rant]
Obviously I'm a little miffed.
So, that shift I picked up a chart and was positively beaming when I saw it was a pt in for IVT who needed a new line put in. So I hustled in there and got all set up, grabbed one of the senior RNs to observe me, got allllll prepped and then....
Tourniquet on.
Examine arms. Nothin'.
Dangle arms. Warm compress to arms. Nothin'.
Except.... the RN peers over my shoulder and points out one tiny thready vein over the patient's knuckle. My very first stick - this could be it! I grab a 22 and try not to sweat onto my patient as I hover the ONC... take aim.... GO GO GO!! And I went. Flash in the chamber and I attempted to thread it and.... nothing! The catheter stopped dead like it hit a wall. Or a knuckle.
Pasting on a smile I deferred poke #2 to the RN. To my relief, though, she also had a lot of trouble finding a good vein - it wasn't just me! That pt took about 5 pokes before we got her with a 24.
That was it for my tries that night.
Sunday morning I'm back in the ER and I told everyone that I was ready to get my 3 starts!!
So the charge RN grabs me at about 1100 to start a line on a guy who was in for severe abd pain. She gives me a 20 and I get to vein hunting. I find a decent one on the back of his hand and prep for the insertion. I am positively STRESSED, though, because the guy was writhing in pain and anxious++ about getting the stick. I'm stressed because he's watching, his wife's watching, and the RN (a very intimidating woman with no real tact filter) was hovering over my shoulder giving very very precise instructions and I just about stroked out from the pressure. I go for the stick and he is actually kicking his feet on the bed. I feel pretty much as bad as can be felt because I can't get the vein. I don't want to be "THAT nurse", the one who fishes the needle around, so I give it about 2 more seconds and I pull the needle out. The RN says she'll take over and she gets a line in. She then yells out and asks one of the RNs to help me do an ECG on him.
That pretty much did it for me. I'm quite confident with ECGs. I do at least 5 of them a shift. So, shellshocked and fighting back my feelings of inadequacy, I "help" the other RN get the leads on him and then bail out of there before I do something embarrassing like cry on my patient.
The charge RN calls me up to the desk - "I need you to document the unsuccessful starts." As I'm standing there, reeling from the overwhelming emotions from the last 15 minutes, she began critiquing my IV attempt. "That's not how WE learned it in school," she says, and I kind of croaked out an answer while trying to keep my cool. She kept critiquing my approach and then one of the newer grad nurses caught my eye with sympathy and that pretty much did it. Yup, I started sniffling, and then a wee tear escaped my eye, and then the emotional dam burst and I got all kinds of upset.
The charge kind of gave me a side hug and told me I'd get it next time, and to go sit down in the back and collect myself. So I went, to try and pull myself together.
But I wasn't upset that I didn't get the IV. It wasn't that at all. It was this overwhelming sensation of being completely UNETHICAL - here I was, barely a full day out of the IV lab with a mere 2 starts on my young male lab partner with great veins, and essentially PRACTICING on patients. Really, that's what it was (and is). I don't know what I'm doing, so I'm practicing on human beings, and it HURTS them, and that's what bothers me most of all. I am hurting people in my attempts to learn. I am more okay with it hurting AND a successful start, but to hurt people like that and to miss the vein.... wow, I hate that so much.
Don't get me wrong. I do completely understand that the only way to learn this skill (and any nursing skill, really, but this is kind of the Big Deal) is by practicing on anybody and everybody. Nobody was born knowing how to thread an 18 into a capillary (I jest ;) but it just really bothers me that my learning is coming at the expense of someone's well-being. More or less. You know what I mean?
I just wish there was a way to get real experience without real people. Those dummy arms are a joke. They help you get the psychomotor action of retracting the needle and applying Tegaderm but that's about it. The "skin" is riddled with holes, the "veins" are rigid and approximately the size of fire hoses, and there is no traction required.
So I was quite emotional from all of these thoughts, plus the incident with the charge, plus another incident that morning where I'd sent a female pt to xray before her preg results had come back (not entirely my fault, plus what the hell does BRV mean, but I still felt awful and had these pictures in my mind of a 17 year old boy with severe deformities because I'd sent his mom to xray without realizing he existed). The results were negative. But still.
Nursing is a tough job. Emotionally tough. There really aren't that many jobs in the world where if you made a mistake, any mistake, someone is instantly and often severely affected. Even if you had no idea you were making a mistake (like how I did not think to check the chart for other orders before I took the pt to xray), BAD THINGS can happen. And they can happen to good people, be they patients or healthcare providers.
Anyway. After all of this went down, all I wanted was for 1530 to come so I could go home and forget this day ever happened.
I was charting when someone tapped me on the shoulder. I turned around to see Michelle, one of the younger nurses on the unit. I'd been buddied with her before and found her to be kind, knowledgeable, and pleasant to be around. She beckoned me into the clean utility room and gave me a great big hug.
"I understand how you're feeling today. We've all been there. But you can do this! You CAN start an IV! You WILL start an IV! And you will be good at it! In fact, it is my personal mission to get you an IV start before I go on holidays."
We discussed my technique and what I was doing wrong. Michelle thought I was blowing the veins by going in at too steep an angle. "But school said we should enter at 45 degrees until we hit the vein, then drop down to 15 degrees to thread it?"
"Forget that!" she laughed, "I almost ALWAYS go in at a low angle, especially those superficial veins."
It was pretty close to the end of the shift so I didn't think that would happen. However, 1500 rolled around and Michelle was waving a chart at me from across the unit. "Do you want to try?" she asked excitedly, "it's an 80 year old man!" She handed me a 20.
Wow. A 20 gauge in 80 year old veins. And with my 6-inch-tall confidence and emotional lability.
"You can do it!"
I walk in the room and find the guy there with his wife. Michelle is right behind me. She's offered to smoothly swoop in if things don't look like they are going well.
Tourniquet on.
Examine arms.
HOLY SMOKES there are ropes of blue up this guy's arms. I feel like I could thread a gauge the size of my pinky in there. Confidence surges briefly. Here we go....
Patient starts muttering that he hates needles. Wife tells him to suck it up.
I aim the needle at 45 degrees, catch myself, and drop it down to 20 or less. One, two, three, POKE! GO GO! I hit the vein right away. I remember to push the needle in a tiny bit more and then thread the catheter, which slips right in. We draw the labs. The vials shoot full of red. We hook up the line and run the bolus, which drips rapidly in the chamber. It was a good one!!!! :D :D I have to stop myself from beaming at this guy and dancing out of the room because I am SO glad that I got my first IV on a real patient on the same day as my bad experience.
So Michelle, although you'll probably never read this, THANK YOU.
For the record, I've had more failed attempts than successful ones, but I've now started 5 IVs, and all the ones I started I got on the first poke. It's getting easier, especially now that I can start them independently. I remember a post I was reading on allnurses to help me get better at IV initiation. One nurse said that when she was working, she told everyone that she got the first 2 pokes on every patient to come in the doors. She didn't shy away from the scary ones because how else was she going to learn?
Truth.
IV Start Lab
-- from the cellular desk of undergrad RN
Blogroll Update
2 hours of hand coding later, it has returned, and better than ever!
Check it out for some good reads, if you're having a chill weekend and need something to do :)
Maybe I learned something in Psych after all
Immediately, sez I, "CONVERSION DISORDER"
25 minutes later, after all the exciting build-up of symptoms and escalating drama...
Yup, it was conversion disorder.
Here I thought I forgot everything from Mental Health!
Speaking of mental health, I summoned every ounce of courage I had and volunteered to do the admission for someone who was suicidal the other day. It was optional for me but one of the nurses encouraged me to go for it.
Even in my Psych rotation I never asked anyone if they were suicidal.
It truly wasn't the difficult conversation I thought it would be. Patient was an older lady, landed immigrant, here for 30 years, her only family was her husband and children. She missed her extended family, missed "back home".
I just kind of winged it but I asked her lots of questions about her mood lability and got her to rate her emotional intensity. Then I asked if she ever thought of hurting herself or anyone else when she felt like her emotions were out of control. She answered in the negative and we moved on in the assessment.
If she'd have answered yes, my next question would have been "do you have a plan?" and we would proceed from there.
Honestly, the hardest part about the question of Are you suicidal? is asking it.
Rapture?
Being at the window facing the waiting room, of course, means that I am that I am the prime target for those asking how long the wait was going to be. I'm still trying to find a way to say "a long time" or "hopefully soon" without actually telling them a TIME because that's when they will be coming up to the window thinking they are going back. And unfortunately the back was full of really sick people who weren't going anywhere.
I call up one girl to the desk for reassessment and she is doubled over in pain, dragging her feet, arms over her tummy. She sits down and I reassess her vitals. Abdo pain is increased since arrival. Feels nauseous. Has not vomited. She had to wait quite a while to get to the back, because of the dearth of beds.
So a while later, I am zipping around cleaning rooms and I walk by hers.....gown on the bed.
"Wha?" I said, possibly out loud. I don't remember her being discharged. I go to the computer and she is still showing as admitted.
Mystified, I go back to the room to make sure she hadn't gone to x-ray or something. Nope, gown on the bed, and hey, is that her IV ripped out? Yes, yes it is.
Has the rapture come and stolen her away? She seemed to be really in pain. I asked a nurse who said she'd gotten a morphine shot and her kids were fighting so she decided to go home. Without being discharged? Okay...
In other news, last night was the night staff started calling me out on mistakes. Which is good, and all, but I felt a little blindsided because they were things no one had previously told me about.
For instance I was asked to bring some people back and I wrote them up for the chart. But I didn't start nursing notes on them because I thought that was done by the nurse on that team. So picture my surprise when I am in the middle of a dressing change and a (fairly intimidating) nurse comes up to me and asks where so-and-so's nursing notes were, because he'd been back for a couple hours and they needed to chart his vitals. Then when she learned I hadn't started them, she walked away saying "bad nurse, bad nurse". Unfortunately there was a little kid also sitting there who then asked her mom what "bad nurse" meant. Umm..
Then the charge saw me and told me I needed to start nursing notes on all the patients I brought back, because so-and-so was a Triage 3 and he was being transferred out, and he hadn't had vitals done in however-long. I think my cheeks were a new shade of red.
Later, I was sitting at the reassessment window and a guy comes in with a kid. I see the kid and he looks pale but alive. Dad says "hey, my kid's having an asthma attack". I pause, at a loss for what to do. No one has told me what to do or who to call if this happens. The triage nurse is busy with another person and the last time I interrupted the triage nurse (a different one) with someone who was worried, she told them to sit down and wait for triage. So I told this dad the same thing - just wait in the chairs and the triage nurse will assess you. The dad kind of glowered at me but they went and sat down. Then the kid got triaged a few minutes later satting at 88% with decreased air entry, tripodding, and in-drawing. Oh my gosh I felt so bad. I talked with some of the nurses about it later and they said that there was a sign for SOB/chest pain to report immediately at the window. The kid was admitted quickly and stayed back for pretty much the rest of my shift. I was also quite humbled because when I looked at the kid briefly, he looked fine to me. I obviously have a lot to see and learn about kids and SOB in general.
Then I was asked to bring another person back who was a ?cardiac patient with history of stroke. I did her ECG, brought her back, put her in the room they told me to, put her on the monitor, wrote up her chart, AND yes I wrote up her nursing notes. Then, a few hours later, a different fairly-intimidating nurse comes up to me and says hey, you need to report off to one of the team members when you bring someone back. What if she crashed and we didn't know what was going on?
So again, I felt like I screwed up without knowing that I was screwing up because this wasn't something that they really emphasized in my buddy shifts.
So I learned last night that it is better to communicate TOO MUCH than NOT ENOUGH. Tell at least 3 people what you're doing, and possibly also the charge nurse. Don't feel bad about interrupting, when necessary, because the alternative is not good.
Lessons learned in the ER.
Friday Night in the ER
- a very large woman with a nasty wet cough satting around 85% on room air (her chest x-ray was almost white)
- a frail grandma who had just finished radiation for cancer, who came in at midnight because she couldn't sleep and felt nauseous
- a kid who'd been maced (by security?) at an event
- a guy with inverted P waves admitted for stabbing chest pain - turns out someone placed the ECG leads wrong, he was fine with some Toradol
- a young couple and their weeks-old babe with diarrhea
- a gangbanger who punched through glass instead of his girlfriend, but seriously sliced his arm just proximal to the medial epicondoyle - deep lac was about 4 inches long and gaping about 3 inches wide - the police found him by following the trail of blood down the street
It was hopping in the ER. I was running ECGs back-to-back, taking specimens to the lab, and herding someone's 5 children under the age of 10 that she decided to bring with her to the ER without extra supervision. One of the docs left at 0300 so we were down to just one doc until 0600 and of course that's when things started to get hairy. Our nurse at triage decided to hang out in the back and keep an eye on triage using the security cameras, because all of the people with sore throats and vomiting in the waiting room kept shooting her death stares.
We had one lady on cardiac observation, the guy with the inverted P waves taking up our peds trauma bed, and another guy came in about 2 weeks post-CABG with crushing chest pain, tachycardia, and a-fib (tachy a-fib? or is it just that it was reading the extra atrial beats as the actual pulse rate? forgive me, cardiology nurses, for I know not what I don't know!), the gangster with the arm lac woke up from his drunken snooze and started howling, the grandma who couldn't sleep still hadn't been seen, the kid who got maced needed a shower, all 5 of the loose children started getting tired and cranky, and the young couple thought we were ignoring them and kept hovering around the desk with babe in arms.
So despite the madness of those three hours, I rolled with it, because the staff were so awesome to witness. This wasn't their first barn dance. With one swoop, the nurses got the kids cozy with some coloring books, told the young couple that they WOULD BE SEEN but not NOW, got the maced kid into the shower, buried grandma in 5 warm blankets (and lo, she fell asleep!), soothed the gangster back to sleep until he could be seen, and all of a sudden the charge nurse pulled me into the other trauma room and said "watch this".
The guy with a-fib was just signing his consent for conscious sedation and attempted cardioversion. They placed the electrodes sandwich-style on his left chest and back, snowed him with fentanyl and propofol, and set the current. Then the physician gave the go ahead. The nurse called CLEAR and made sure we were all back before pushing the shock button. The guy went rigid and then limp.
"Owwwwww," he groaned, motioning to his chest.
We all watched the rhythm as it settled into normal sinus for a few beats....and then blip, blip, blip-blip-blip his heart rate climbed back up to 140 and we saw the beats become irregular again.
The physician ordered a higher electrical current. ALL CLEAR! Shock given. Normal sinus, and then a-fib.
Again, higher current, shock, normal sinus, and then a-fib.
The physician decided to discontinue the cardioversion and instead just hold the patient until he could be admitted to cardiology in the morning.
A couple of hours later, the new doctor was coming on so I pulled someone out of the waiting room for the first time in hours. I looked in the chart. Sore throat x 3 weeks with slight cough, no fever, nontender palpation of lymph nodes. Came in at 0300 on the Saturday of a long weekend (and waited 3 hours) for....what, exactly? A throat swab and dispo with abx...
And then it was 0700 and the gangster was getting his arm stitched up. I played doctor's helper and held the pt's arm in an awkward superman position, while also running to grab sutures and stuff since, although the doc had the suture cart right there, he had managed to turn it so I couldn't get into it, and he was sterile so away I went. It was worth it though because it was awesome to watch him pull the lips of the lac together and get it sewn up. There was a large vein that had to be tied off. He started in the middle of the lac and guessed where to start sewing. After a couple of false starts he got it evenly joined and worked his way out to either end, and then filled in the gaps. All together I think there were 10 sutures. It was neat to watch him pull the edges together , all the subcutaneous fat kind of popped out and sqooshed all over the place. Once he was done, it looked amazingly clean. Especially considering the amount of blood I'd washed off his arm, and how much had caked onto his pants.
I applied a dressing of adaptic, 2x2s, 4x4s, and cotton wrap. Then the oncoming day nurse told me to go home.... so I did :)
*Pinches self* I can't believe I get paid for this. I LOVE EMERGENCY NURSING!
Captain's Log: First Night Shift
-- from the cellular desk of undergrad RN
First day in Emergency Externship
So for anyone who hasn't had exposure to emergency nursing before, I will try to elaborate what the flow is like. This particular ER doesn't assign specific patients. They have recently implemented team nursing, so a bunch of nurses will be assigned to a wing and work together to meet the needs of all of those patients. My preceptor was assigned to float between the two teams, as well as cover charge and triage for breaks.
My shift started at 1530 and we took report from the off-going charge. I noticed that the report went very quickly, identifying only the chief complaint and how long they'd been there, and any labs that needed to be drawn.
We toured the unit and she pointed out all of the equipment in the different rooms. I've been volunteering on that unit since November but it was cool to see it through fresh/knowledgeable eyes. There is a minor procedures room, orthopedic casting room, EENT (eyes, ears, nose, throat) exam room, 4 stable beds, 4 fast track beds, 4 monitor/observation beds near the desk, 2 gyne/peds rooms, 2 trauma/resuscitation rooms, 1 reverse isolation/positive pressure room, and 1 secure room with superstrength door and optional camera monitoring.
 |
| morganlens.com |
Like a lot of you, I think, I have followed a ton of emergency nurse blogs since well before nursing school in 2008, including those of the illustrious Nurse K, Girlvet, and NNR, newer ones like newnurseinthehood and Maha, and newer-to-me torontoemerg. Like you I have uttered many a guffaw and/or facepalm at the stuff people do to end up in the ER at odd hours when other people, such as myself, would much rather be home in bed. I am (pleased? saddened? resigned?) to report that I saw several examples yesterday in one shift alone that amazed me, especially in terms of my rosy nursing school glasses.
My next admission was a young man with throat tattoos (listen, I LOVE tattoos. I have two large ones myself. But I have never seen a throat tattoo that I didn't immediately associate with Tapout) dressed head to toe in Ed Hardy who came to visit us with a migraine. Okay, I've had migraines as a teenager. All I could do, once I got the visual disturbance aura, was get home ASAP so I could lie in bed in dark silence and barf my guts out while praying for it to be over. Seriously, the ED is the LAST place I'd want to have a migraine. This young man did not exhibit any of these symptoms. I'm not sure what he got discharged with, but I think he waited a while.
 |
| San Francisco General Hospital |
Another interesting thing was a little boy who had stuck a not-so-little bead up his nose. I have never worked in peds before outside of postpartum and preschool participatory observation for a few days. I had no idea what they would do. The RN grabbed him and wrapped him in a full-size swaddle, pinning first one arm and then the other as they rolled him tightly into a sheet like a little sausage. I helped to hold him still as the physician tried to excavate the bead via suction. No dice, but one of the nurses found a metal tool that bends at the tip when you press the trigger and they threaded that through the bead. Success! I was amazed at how big it was. Wonder how it fit up there in the first place!
A few other things I saw -
- The ortho tech showed me how to do a wrist assessment to help decide which carpals were affected, and determine which x-rays to order
- Nancy starting IVs so fast she made it look easy, and I was consumed with envy
- A roughed-up prisoner who got into quite the scrap (I've never seen someone look that, well, beat up before)
- A little baby with a case of Grade A diaper rash
- Oozing shingles pustules
- An ECG on a woman with a heart condition and chest pain - she was graduated to an observation bed. Her husband peppered me with questions about why she was getting a N/S infusion and why they ordered what tests they did, and, MOST importantly, how long they would have to be there. Apparently there are places more important to be than in the hospital ruling out MI...
- Query fish bone stuck somewhere deep in a guy's upper GI, not sure what they did with that one
- Nancy also volunteered me to admit a query anaphylaxis reaction. Lady had hives on her tongue and reported throat closure/swelling. I was pleased when my brain suggested I auscultate and listen for evidence of decreased air entry. So I busted out my stethoscope and listened to her perfect breath sounds all the way down to the lower lobes. Nancy approved of this and had me chart it. I think my hand shook a little as I signed my new designation, haha :)
I saw way more things in one day that I saw in weeks at clinical. I seriously loved it, every minute. I was also super grateful for the extremely kind staff who were more than happy to show me cool things and ask me tough "thinky" questions.
I can't believe I get paid for this!!! I would have been there for free. Wait, don't tell that to my boss..
Can't wait for my next shift tomorrow :)
1st day on the floor in Emergency
I have also just started taking SOCI 271, Intro to the Family, during the spring session at school, as credit for my senior elective. I am SO THRILLED to report that I have begun my 4th Year courses!!!
(I also love spring session because it's 3-hr lectures, 5 days/week, for 3 weeks. Bliss.)
I think my brain exploded
We spent 7 straight hours going through (literally) STACKS and STACKS of HR stuff, paperwork, and all kinds of tips and tricks for assessing different populations and situations. I have 3 stuffed folders and I think I will take some time to organize them into binders because they seriously gave me some of the best reference material I've come across since starting school - and free!
Orientation was provided by the clinical nurse educator, herself a very knowledgeable ER nurse with floor experience in critical care, trauma, and flight nursing. It was like my assessment course and my acute care course plus lots of extra information all rolled into one day. I was on learn overload. I am SO excited to see this all in action.
I also saw educational videos on some kind of contact-looking-thing that fits over the eyeball and hooks up to NS to flush the eye of chemicals or debris, and how to install/use an intraosseous (IO) infusion set. Then I played with the drill. No needle ;)
So my next step is to book my buddy shifts (2 days, 2 evenings, and 2 nights)... and then after that?? I don't know yet. I don't think the unit manager knows yet, either. It seems like a gongshow-kinda place. I think I've been spoiled for the last 5+ years I've been in quiet offices with orderly HR and management processes...
I sent an email to my other job letting them know what days I was free. I shall see what they say. I am looking forward to not working there anymore, but prudent thinking suggests that I will benefit from working so much this summer, and I can quit with a clear conscience and a full bank account for the Fall term.
Procrastinating
Since Zazzy asked, I'll define UNE - "undergraduate nursing employee" is my province's designation for a 3rd year student nurse; since BSN was made entry-to-practice for RNs in this country, it's how we can get paid experience working in an RN-type role before we graduate.
The UNE position does not fall under the auspices of our regulatory college or union; rather, it is a protected position that is only available to regular-entry BSN third year students (not LPN-RN bridging students, or accelerated BSN students) and it is designed to be temporary (cannot work full-time for more than 3 months, less a day, per UNA guidelines - this is to make sure that a UNE does not take the place of an RN or LPN position).
The UNE takes on a lighter load than an RN, with lower acuity, and is responsible for patient care for anything he or she has been trained to do already in school. For example I can do anything I have done in clinical before - foleys, wound dressings, IMs, bladder scans, etc. Things I have not done before I can watch and learn, such as placing NGs. Things that are outside of my clinical scope I cannot do as a UNE. Such as IV push meds or defibrillation - which is totally okay, I'm in no hurry for that kind of responsibility.... lol
Otherwise I function in my full clinical scope. I can do planning, teaching, skills, and nearly everything an RN would do. I'm not totally sure what I *can't* do, yet, because I think that's probably specific to the type of environment I will be working in. I've never had a rotation in Emerg, or spent any significant time there outside of my volunteer position (which never exposed me to much except where the supplies were, really). It won't be like my med-surg experiences with paging the docs and stuff. I like this particular environment because the nursing station is combined with the physician desks. It will be an excellent opportunity to learn by eavesdropping on everybody, especially because curtains aren't particularly soundproof! :)
So yes, I will be working 0.5 FTE from May through August (that's about 20 hours a week) and mainly evenings and nights. I have never worked overnight before. I've worked late-as-hell (6 PM to 2 AM) and early-as-hell (6 AM to 2 PM) but never crossed that barrier. If you have any tips please share. I am concerned that I will turn into a surly, cheerless, friendless prickle. My plan to also work 3 days per week at my desk job, likely in midmorning-afternoon, kind of hinders the idea of turning full-on vampire. I'm not sure how this will work out. If something has to give, I will stick with Emerg.
Oh! That reminds me. I was going to write up some of the interview questions in case that helps any of you out in the future. I have them scrawled on a notepad somewhere...
At any rate, as per the title of my post, I am technically supposed to be writing a ten-page critique of a research report right now. It's a self-imposed deadline for the research class I'm taking by correspondence. Knowing myself and how I am, I booked the final well before I finished any of the projects, so that I would HAVE to finish it. So now I HAVE to finish it, or fail the course, by Thursday April 28............ but it's only the 17th, and of course you see my temptation :)
Before I get back to the
Yeah! Bet you thought I was done, based on the crappy posting of late...
Nope, I am 4 weeks out of 5 from being finished my Community/Public Health rotation.
Tuesday is our oral report about the agency placement with the preschool kids, and our teaching plan re: toothbrushing and washing hands. Wednesday is our actual presentation to the kids. Thursday is our final evaluation, and Friday is a long weekend, my last before I go back to work.
(For the record, I took a leave of absence from my desk job for the months of March and April in order to focus on clinical, and it was the BEST THING I EVER DID for myself in school. Hands down. Last year my hair was literally falling out. This year I am able to attend my horse-riding classes, work out, make healthy food choices, take on 2 correspondence classes, AND do a decent job on my clinical projects)
In regards to Community Health, well... I have felt like I could fit into every clinical placement I've had so far. Even postpartum which I honestly thought I would hate (thanks CC for helping me consider otherwise :)
But, man, Community Health has absolutely NO appeal to me. It could be that I've worked desk jobs for about 6 years now and I'm numb to the pride I once had about having my very own cubicle. I can't stand office work or office gossip. I hate photocopiers and water coolers and I REALLY hate getting emails from people who don't know what Reply All means. I realize that there is a hands-on component in public health, i.e. when you actually go out and assess babies or teach college kids about STIs or do an immunization clinic for Grade 5 kids.... but that seems to be only 10% of the job. The good 10%, IMO. The other 90% of the time seems to be spent in the office, trying to round up resources and liaise with other people and hammer out meeting times and set up appointments, etc, etc.
Maybe CHN/PHN will be appealing to me when/if I have family responsibilities or am tired of running around all day.... but for now, get me back in the hospital, stat.
I shadowed one day last week in the Hip & Knee Clinic, where people go for pre- and post-surgery teaching and assessment. It was actually a really cool experience, especially given my rotation in Orthopedic Surgery last year. I got to take out some staples and do a dressing change. Compared to the rest of my rotation, it was practically critical care in there! lol!
Okay okay, I'm going to go write a paper now. Honest....
Undergrad RN, UNE
I went in there and blew their minds with my clinical genius!
Okay, I was pretty nervous but very prepared.
FYI - I read a tip about putting baby powder on your hands to prevent clamminess. I suffer from seriously sweaty palms when I am under the microscope so I tried it. It worked very well. No one got grossed out by shaking my hand for a change...
At the end of the interview, they offered me the position, on the condition that I am:
A) not a criminal, and
B) not lying about being a nursing student
So orientation's on April 26 and 27!
Unfortunately the position (like every freakin' position in this province) is only a 0.5 FTE. So I will also be keeping my regular job for another summer. Still, who cares! I get paid to go to clinical! :D
I have been waiting for this opportunity since before I started nursing school. I remember Googling like crazy to learn about what it meant to be a student nurse in this province. I found the UNE position and told myself - that's what I want to do in my 3rd year of school. And here I am!!!
This is a great day!
UNE Interview in T-1.5 Hours
My hair is done. My clothes are pressed. I am wearing my STTI pin for awesomeness.
I am browsing my blog archives to try and remember some of my more influential nursing moments.
..........and I am freaking out!!!




